What is COVID-19
Coronavirus disease 2019 (COVID-19) is a respiratory illness that can spread from person to person. The virus that causes COVID-19 is a novel (new) coronavirus that was first identified during an investigation into an outbreak in Wuhan, China.
COVID-19 has been spreading from person to person all over the United States and the world, and your risk of infection is higher if you have close contact with someone who has COVID-19.
UnitedHealthcare Response
The purpose of this blog is to help you understand the steps that UnitedHealthcare is taking to help us through these hard times.
If you are a member of UnitedHealthcare (Medicare Plans, Employer Group Plans, Medicaid Plans, etc.), and you have questions about your benefits, it’s best to call the phone number listed on your UnitedHealthcare ID card.
You may also sign into your health plan account at https://www.uhc.com/sign-in.
One of the most recent announcements made on April 7, 2020 from UnitedHealthcare was their commitment to accelerate $2 Billion in payments and financial support to health care providers. Their goal is to help address the short-term financial pressure caused by the COVID-19 emergency.
Their move to accelerate claim payments to medical and behavioral care providers applies to UnitedHealthcare’s fully insured commercial, Medicare Advantage and Medicaid business.
The financial support currently includes the provision for up to $125 million in small business loans to clinical operators with whom OptumHealth is partnered.
This decision to provide financial relief to providers builds on previously adopted measures taken by UnitedHealth Group to streamline processes for health care professionals and facilities as well as to help members more easily access the care they need.
On a more personal note, UnitedHealthcare is expanding access to care for its members and has shared new resources they made available.
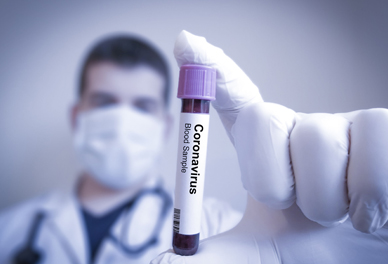
Testing and Medical Care Related to Testing:
In addition to continuing to waive costs for COVID-19 testing provided at approved locations, UHC will waive copays, coinsurance and deductibles for visits associated with COVID-19 testing whether care is received in a physician office, urgent care center or emergency department for all Medicare Advantage members. Any additional coverage for treatment for COVID-19 is administered according to benefit plans including applicable cost sharing.
Medication:
Eligible members needing help obtaining an early prescription refill can call the customer care number located on their medical ID card.

Virtual Care for Highest-risk Members:
UnitedHealthcare is rapidly expanding access to their personalized digital platform which is available on their member website for those who need it most. The interactive platform provides the most up-to-date information about prevention, coverage, care and support needed to rapidly assess symptoms, schedule an in-person or a telehealth visit with your provider, talk to a nurse, refill or schedule home delivery for prescriptions and access 24-hour emotional support.

UnitedHealthcare is also deploying new technology solutions and have established navigation support programs for members who are under home isolation due to COVID-19.
In addition, UnitedHealth Group has committed an initial $50 million investment to fight the pandemic and to help support those disproportionately affected by the outbreak, including health care workers, hard-hit states, seniors and people experiencing food insecurity or homelessness. They are also matching employee donations, dollar for dollar, to support the COVID-19 response efforts.
UNDERSTAND WHAT’S COVERED AND HOW TO GET CARE.
UnitedHealthcare is waiving cost-sharing for members’ treatment of COVID-19 until May 31, 2020 for Medicare Advantage, Medicaid, Individual and Group Plans that are fully insured. If you are a self-funded customer, UHC is willing to implement a similar approach on your behalf.
From now until June 18, 2020, UHC will also waive cost-sharing for in-network, non-COVID-19 telehealth visits for the same plans. This will ease the burden on doctors’ offices and hospitals for non-COVID-19 related visits to free up resources and space for those patients that need priority care.
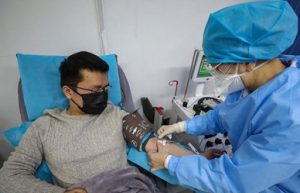
If your provider agrees that you need COVID-19 testing, UHC will waive cost-sharing at any CDC approved testing site during the national emergency.
Only a health care provider can order testing for COVID-19, so if you feel that you need a test, be sure to talk to your provider and have them follow proper procedures.
UHC is also waiving all cost-sharing for any COVID-19 testing-related visit. This includes visits to a provider’s office, an urgent care center, an emergency department or a telehealth visit. This special coverage applies to all Medicare Advantage, Medicaid, Individual and Group health plans.
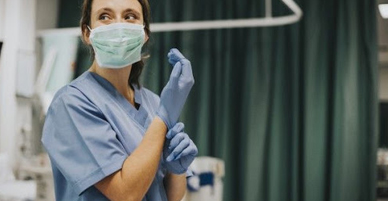
HOW TO GET TESTED FOR COVID-19
For those that feel that they may have been exposed to COVID-19, or if you have symptoms such as a cough, fever, or difficulty breathing, call your health care facility right away.
Do not go to the facility until you have been given proper instructions from the health professional. This will reduce the chance for others being exposed. If your health care provider feels that you will need to be tested, let them order the test for you.
Your provider will give you instructions and will work with local and state health departments to coordinate where you will receive your test.
ADDITIONAL RESOURCES
UnitedHealthcare has expanded services and resources for your support if you are already a member.
Telehealth
UHC has expanded access to telehealth services and it can be used for both COVID-19 and non-COVID-19 health care concerns. If dentistry is covered in your plan, UHC has also implemented a tele-dentistry visit for urgent needs.

Nurse
You can always call the number on your member ID card and reach a nurse if you have questions about your risk, or if you are looking for advice and support related to COVID-19. And of course, you can always ask a nurse about your general health care needs.
Early Prescription Refills
You will have the ability to ask your pharmacy for an early refill on your prescriptions if you have UHC prescription drug coverage or an OptumRx pharmacy benefit. Yours encouraged to check your supply of medications at home and consider which medications you might want an early refill of. Also, don’t forget about Optum Home Delivery, a mail-order pharmacy refill service offered on most plans.

Emotional Health
This is a stressful time. If you find it hard to cope, please talk to someone by calling UHC’s emotional support line at 866-342-6892. It is a free service for anyone. There is also a free on-demand emotional support mobile app called Sanvello to help you cope with stress, anxiety and depression during this pandemic.

UnitedHealthcare is here to help in these times of need. If you have questions about your benefits, sign in or call UnitedHealthcare. Your member ID card will have all the information you need to make contact with them.
We’re here to help! Call us today.







Share your thoughts
Leave your comments