How To Change My Medicare Plan
When you first turn 65 years old, you are in what is called your Initial Enrollment Period. You have a certain amount of time to make decisions on which Medicare plan you want to go with.
But what happens if you are unhappy with the plan choice you made and want to switch plans? Or what about if you move to another town or state?
The good news is that in most cases, you will be able to make changes to your Medicare plan at various times throughout the year if certain things change about your situation.
Initial Election Period
If you are brand new to Medicare, you are in what is called your Initial Election Period (IEP). Your IEP starts three months prior to your 65th birthday month and ends three months after your birthday month (for a total of 7 months).
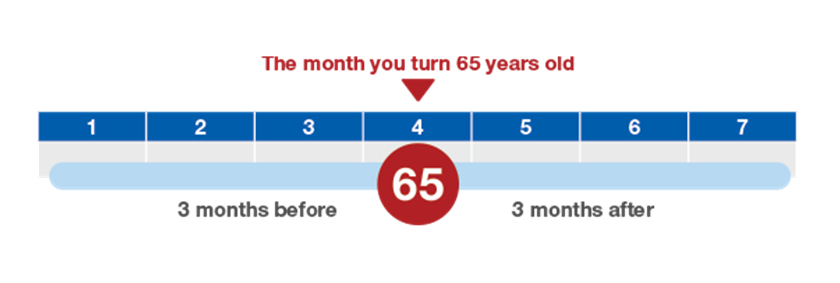
During your IEP, you can enroll in original Medicare (Parts A and B), as well as choose a Medicare Advantage (Part C) Plan and/or a Prescription Drug (Part D) Plan.
There are several choices to choose from, and your options will vary based on the county you live in. It is highly recommended that you speak with a licensed Medicare broker that can help you navigate the various options and explain the differences between those options.
In addition, you may also want to consider a Medicare Supplement
Medicare Supplement Open Enrollment Period
Medicare Supplements have a slightly different enrollment period. This enrollment period starts the first month that you are age 65 and lasts for 6 months. This is an important enrollment period because it is the time period in which you have guarantee issue rights (you cannot be denied coverage) for a Medicare Supplement.

If you miss your open enrollment period for Medicare Supplements, you can apply anytime. The only negative to this is that you are not guaranteed to be accepted.
The plan will require medical underwriting and could deny your coverage, or charge you a higher premium based on your health history.
So, if you are leaning toward a Medicare Supplement over a Medicare Advantage plan, your time for guaranteed lower rates is during Medicare Supplement Open Enrollment.
Changing Plans
Most people will keep the same Medicare plan year after year, especially if you are on a good plan. This is another great reason to have a local Medicare broker that really understands how well these plans perform.
Your broker will help you get in a plan that best fits your needs. But over time, your healthcare-related needs will change. In addition, plan coverages and costs can change from year to year as well. So, you may need to change your plan.
In most cases, the time to change your Medicare plan is during the Medicare Annual Enrollment Period (AEP). But there are other events throughout the year that may open what’s called a Medicare Special Enrollment Period (SEP).
If you are on a Medicare Advantage plan, you also have a 1-time “correction” period known as the Medicare Advantage Open Enrollment Period (MA-OEP). Clear, right? Let me explain the details of each:
Annual Election Period (AEP)
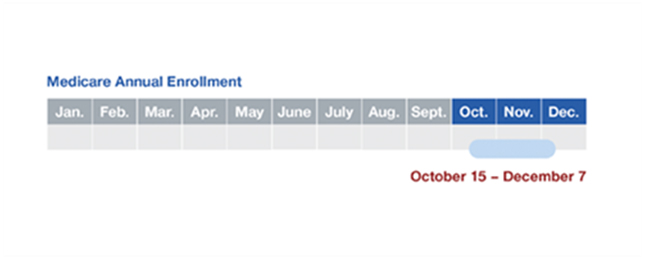
Medicare Annual Enrollment occurs every year from October 15 – December 7.This is the time you can change your coverage choices if you want to. Changes made during AEP take effect on January 1 of the following year. If you are happy with your current plan, you do not need to take any action during AEP, your plan will simply renew automatically at the start of the new year.
Each year, your current plan will send you a document called the Annual Notice of Change (ANOC). The ANOC explains any plan changes that will go into effect at the start of the new year. It is important to review this document so there are no surprises. You can also call your broker to help you understand your ANOC if things are unclear.
Here are the changes you can make during Annual Enrollment:
- Enroll in a Medicare Advantage plan for the first time.
- Drop a Medicare Advantage plan and go back to Original Medicare.
- Switch from one Medicare Advantage plan to another.
- Join, switch, or drop a Medicare Prescription Drug plan (Part D). Be aware that you may be charged a late enrollment penalty if later you decide to join a Part D plan again.
- Annual Enrollment is also a good time to enroll in a Medicare Supplement plan from a Medicare Advantage plan. It gives you time to make sure you will be accepted by the plan before you must make a final decision.
Medicare Advantage Open Enrollment Period
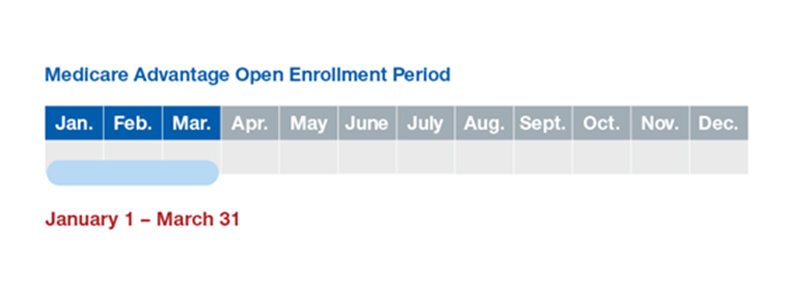
The Medicare Advantage Open Enrollment Period (MA-OEP) allows you to make a one-time correction/change to a different Medicare Advantage plan, or simply drop your Medicare Advantage plan and go back to Original Medicare. The first rule with this election period is that you must be enrolled in a Medicare Advantage plan to be able to make a change. The MA-OEP happens every year from January 1 – March 31.
Medicare Special Enrollment Period
A Medicare Special Enrollment Period (SEP) is available in certain situations and allows you to join, change or drop a Medicare Advantage plan or Prescription Drug plan outside of the Annual Enrollment Period.
These events are also known as “qualifying events”. For the most part, you have 2 full months after the month of the qualifying event to make a plan change.
Here is a list of the most common events that qualify as a Special Election Period:
- You have moved outside of your current Medicare plan’s service area.
- You are moving within your current plan’s service area, but you have new plan options in the new area.
- You are moving into or out of an institution.
- You are leaving a retiree, union, or COBRA group plan.
- You are losing creditable drug coverage.
- Your current Medicare plan stops servicing your area.
- You are enrolled in Medicaid/AHCCCS, or get extra help for Part D.
There are many more SEP’s that will allow you to make plan changes. Contact a local, trusted Medicare broker who can help you understand all the complex rules.
How to Change my Medicare Plan
This is where it gets extremely easy for you. Contact us!
We are licensed Medicare brokers and we are contracted with all the plans available in your area.
We are experts with understanding how and when you can make changes to your Medicare plan.
We look forward to helping you.
We’re here to help! Call us today.

Share your thoughts
Leave your comments